A diabetic foot ulcer is a common and most devastating complication of diabetes. It is the foot affected by ulceration and neuropathy and/or peripheral arterial disease (a disorder of blood supply) of the foot in a patient with uncontrolled diabetes. The prevalence of diabetic foot ulcers in the diabetic population is 4–10%; the condition is more frequent in older patients.

It is estimated that about 5% of all patients with diabetes present with a history of foot ulceration, while the lifetime risk of diabetic patients developing this complication is 15%. In North India, the complication rate of diabetic foot is 14.3 %.
A diabetic foot ulcer is very problematic and difficult to treat, that’s is why its management involves a multidisciplinary approach like primary care surgeons, nurses, podiatrists, diabetologists, and vascular surgeons, as well as all healthcare providers involved in the prevention or management of diabetic foot ulcers.
What is a diabetic foot ulcer (Facts you should know)
Any disruption or damage to the normal anatomical structure and function is defined as a wound. Some wounds can be just a scratch (a simple break in the integrity of the skin) or they can be deeper, extending into deeper layers of skin which can damage muscles, blood carrying vessels, nerves, and even bone. Diabetic wound management can become very challenging, and you need to visit an expert wound specialist who can understand wound management protocol.
Risk factors for diabetic foot ulcer
Factors which reduce the chances of healing-
- Uncontrolled hyperglycemia (Hb A1C > 8.0)
- Inability to offload the affected area
- Poor circulation
- Infection
- Poor nutrition
Factors that increase the chances of healing-
- Serum albumin > 3.5 g/dL
- Total lymphocyte count > 1,500/mm3
A diabetic foot ulcer can be divided into the following category-
- No open lesions; may have healed lesion.
- Superficial ulcer without penetration to deeper layers.
- Deeper ulcer, reaching tendon, joint capsule, or bone.
- Deeper tissues involved, with abscess, osteomyelitis (infection of the bone), or tendonitis (infection/inflammation of the tendon)
- Gangrene (death of tissues or cells) in a portion of the forefoot or heel.
- Extensive gangrenous involvement of the entire foot.
When caught early, foot ulcers are treatable. Visit a wound specialist if you develop any sore. Early detection of infection can reduce the healing time and cost. Infections if not addressed on time may require amputation.
Ulcers may take even longer to heal if you don’t control your blood sugar levels or if constant pressure is applied to the ulcer.
Remaining on a diet that helps you meet your glycemic targets and off-loading the affected area.
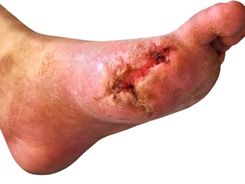
Negative Pressure Wound Therapy in diabetic foot ulcer
Wound management with conventional technique is a difficult task as desired results are not achieved and have always been a cause of concern for treating clinicians. The need of the hour is to develop a newer novel technique that might be useful in the healing of difficult wounds and delivering at par or better results as compared to the conventional wound dressing.
Negative pressure wound therapy (NPWT), a relatively newer technique using vacuum-assisted closure (VAC) shows promising results in the management of difficult wounds. VAC accelerates debridement and promotes healing in various types of wounds by creating negative pressure which is lacking in conventional wound healing treatments. The basic unit of the system is a microprocessor-controlled vacuum unit that is capable of providing controlled levels of continuous or intermittent sub-atmospheric pressure ranging from 25 to 200 mmHg.
How does NPWT work for Diabetic foot ulcers?
1. Drainage of interstitial fluid (fluid in body tissue) decreases localized edema, which increases continuous blood flow and decreases tissue bacterial levels.
2. Application of negative pressure produces mechanical deformation or stress within the tissue resulting in protein and matrix molecule synthesis which enhances faster recovery.
When should you go to the doctor?
- Soft tissue injuries prior to surgery
- Grafting or reconstructive surgery
- Infected sternotomy wounds
- Open abdomen wound management
- Closure of laparotomy wound
- Split thickness skin grafts for burn patients
- Knee amputation
- Acute and traumatic wounds
- Sub-acute wounds (i.e., dehisced incisions)
- Chronic open wounds (stasis ulcers and diabetic ulcers)
- Meshed graft
VAC- The small ambulant unit is recommended for
- Venous stasis ulcers
- Pressure ulcers
- Lower extremity diabetic ulcers
- Lower extremity flaps
- Dehisced incisions
6 steps methods of applying VAC
- The foam dressing is cut to the approximate size of the wound with scissors and placed gently into position.
- The perforated drain tube is then located on top of the foam and the second piece of foam is placed over the top.
- For shallower wounds, a single piece of foam may be used and the drainage tube is inserted inside it.
- The foam, together with the first few inches of the drainage tube and the surrounding area of healthy skin, is then covered with the adhesive transparent membrane supplied. While doing this always ensure that the membrane forms a tight seal both with the skin and the drainage tube.
- The distal end of the drain is connected to the VAC unit, which is programmed to produce the required level of pressure.
- Once the vacuum is switched on, the air is sucked out of the foam causing it to collapse inwards drawing the edges of the wound in with it.
- Fluid within the wound is taken up by the foam and transported into the disposable container within the main vacuum unit.
The time duration for the healing of the wounds is shorter in the VAC as compared to the conventional methods which shorten hospital stay & hospital coast.
Advantages of VAC therapy
- Easy to handle
- Hospital admission is not essential
- Good patient compliance and satisfaction
- East to learn how to maintain vacuum at home, can be applied to multiple cases at the same time and give adequate mobility to the patient.
if it is caught in an early stage, the foot ulcers are treatable. Immediately see a doctor if you develop a sore on your foot, as the infection might increase the longer you wait.
